
Cancer antigens trigger anti-tumor immunity. Unexpected spontaneous remissions of even advanced cancers may be attributed to the development of a spontaneous immune response against tumor cells. But tumor cells learn to escape the anti-tumor immunity. Immuno-oncological interventions prevent this “immune escape” by strengthening spontaneous anti-tumor immunity. Many new immuno-oncological drugs suggest that immuno-oncological expertise should be included in the design of concept for cancer treatment.
What is cancer?
Although much detail has yet to be added, biomedical research today knows, at least on a conceptual level, how cancer develops and progresses into a deadly disease. This, however, does not mean that all questions about the origin of neoplastic diseases are already clear. There are enough gaps in our knowledge to keep the research community busy for many years to come.
Question: What is cancer?
Answer: Cancer is a disease of the genes.
 Mutations in genes that participate in directing cell division lead to the loss of control over cell proliferation. The immune system has the capacity to identify protein alterations caused by mutations in the gene that codes for this protein. Mutated cells, including cancer cells, are detected and destroyed at an early stage of their development by the defense mechanisms of our body. In this way, the immune system probably protects us from cancer for a long time, maybe even decades.
Mutations in genes that participate in directing cell division lead to the loss of control over cell proliferation. The immune system has the capacity to identify protein alterations caused by mutations in the gene that codes for this protein. Mutated cells, including cancer cells, are detected and destroyed at an early stage of their development by the defense mechanisms of our body. In this way, the immune system probably protects us from cancer for a long time, maybe even decades.
But just as with other organs, the capacity of the immune system deteriorates with age; the defense front begins to crumble. The increasing weakness of the immune system allows individual cancer cells to hide from scrutiny. In addition to passively hiding from the immune system, cancer cells develop mechanisms for active protection from immune attacks. Only once this is accomplished, cancer can develop into full-blown disease. The immuno-oncology point of view therefore suggests another answer to the
Question: What is cancer?
Complementary answer: Cancer is the symptom of an immuno-deficiency.
The development of cancer understood as a failure of the immune system to prevent uncontrolled proliferation of mutated cells has only very recently arrived in mainstream oncology. Changing perspectives opens the door to aspects of cancer that otherwise remain hidden. Considering only the cancer cell itself and its genetic alterations as targets for therapeutic efforts has prolonged the life of cancer patients. However, we are still far from finding a cure or at least a way of permanently controlling malignant growth. Immuno-oncology tries to see beyond the cancer cell and understand cancer as a complex tissue. Cancer is not just a pile of cancer cells, but a tissue with a defined fine structure that is critically influenced by, among other things, the immune system.
Immuno-oncology
Immune modulation
Can strengthen anti-tumor immunity, prevent the immune escape, block the shutdown of the immune system.
- Immune checkpoint inhibitors: CTLA-1, PD / PD-L, IDO – prevent an immune response against tumor antigens from being shut down, thus preventing the tumor from escaping the immune system
- Immune stimulation: interferons, interleukins – signaling substances of the immune system transmit the attack commands
- BCG Inoculation – an attenuated bacterium that, when injected into the tumor, attracts and activates cells of the immune system
Adoptive immunotherapy
Substitutes insufficient or lacking protective mechanisms in the immune defense against tumor cells.
- Monoclonal antibodies – block receptors for growth factors on tumor cells, which stimulate cells to divide
- Chimeric Antigen Receptor (CAR) T-cells – genetically engineered killer cells that are capable to specifically target tumor cells
Tumor vaccines
Trigger antitumor immunity or boost an existing spontaneous immune response against tumor antigens. Different methods of tumor vaccination have been developed in the last 2-3 decades, but their efficacy has not yet been demonstrated definitively.
Services
The increasing understanding the interaction of tumor cells with the immune system and the availability of powerful IO drugs for the modulation of these interactions suggests adding IO expertise to a treatment concept for neoplastic diseases. I offer to counsel cancer patients and to assist the attending team of oncologists in incorporating the great opportunities of IO into a comprehensive cancer treatment concept.
- Consultation
- Especially in advanced cancers
- Reports and reviews of the most recent literature
- Visit of and discussions with the therapeutic team & the patient
Who may benefit from IO?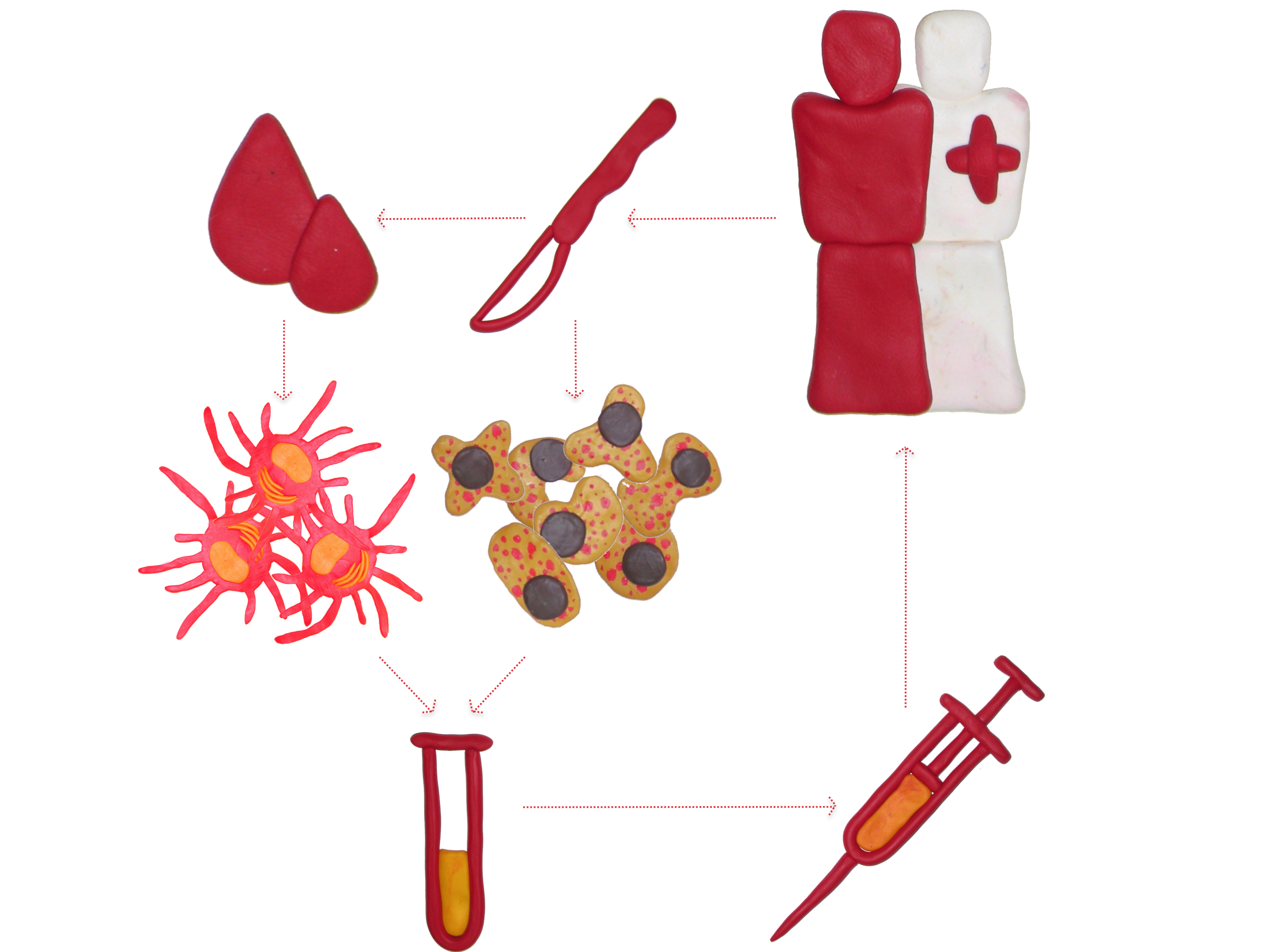
A well-informed off-label compassionate use of an IO drug is a challenge – but also a great chance – in the treatment of advanced neoplastic diseases that failed accepted standard therapy. The great potential of IO suggests that these therapeutics may be used in advanced cancers. The typical patient for a compassionate use of IO treatment has
- Advanced generalized neoplastic disease
- Exhausted all standard therapies
- An advantageous immune status in blood and tumor tissue
What to expect?
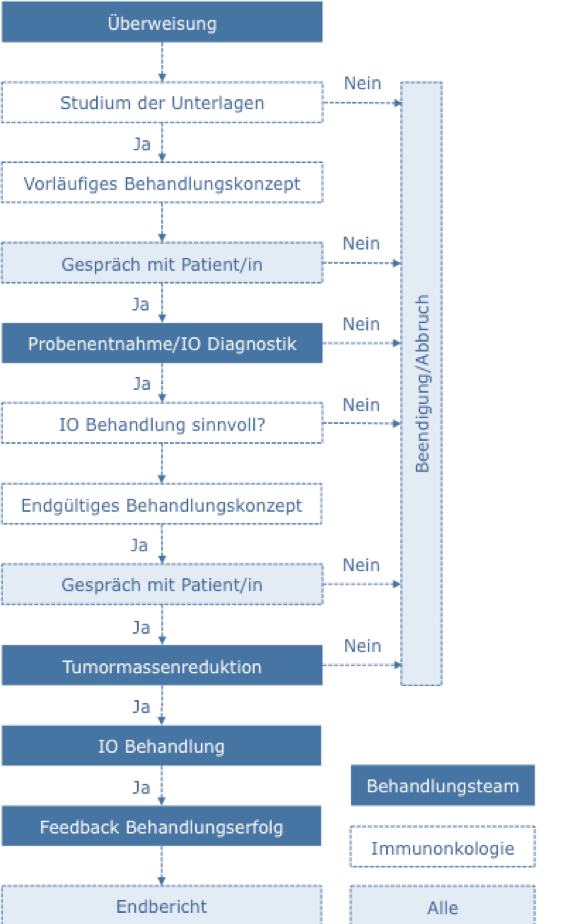
- Proposals for the rational off-label use of IO medicines in advanced cancer
- A unique complementary offer for cancer patients and their families
- If desired, continued IO consultation
Safety and tolerability of IO therapy
The drugs used in IO generally have only moderate side effects. This is of particular relevance, since the deterioration of the quality of life of already seriously ill patients should not be further worsened by an aggressive therapeutic intervention. Immuno-oncology offers the chance of not having to give up cancer patients completely – except maybe for a more or less aggressive pain therapy. As an opportunity for off-label compassionate use, IO may significantly benefit cancer patients in the advanced stages of their disease.
Please note
This service is not intended to replace the medical treatment team. I only offer complementary information and consultation regarding the scientific background of cancer and its treatment. As far as diagnosis and therapy are concerned, you can fully rely on the experience and expertise of your oncologists.

